Case Report
MVP-Induced Ventricular Tachycardia: Paradoxical Role of Implantable Cardioverter Defibrillator: A Case Report
Ronpichai Chokesuwattanaskul1,2*, Mandeep Singh Randhawa2, Randy Ip2 and John H Ip2
- 1Department of Internal Medicine, King Chulalongkorn Memorial Hospital, Thailand
- 2Sparrow Hospital, Michigan State University, USA
- *Corresponding author: Ronpichai Chokesuwattanaskul, Department of Internal Medicine, King Chulalongkorn Memorial Hospital, USA
- Received: Dec 19, 2018Accepted: Jan 03, 2019 Published: Jan 05, 2019
- Keywords: Case report; ICD; MVP; Ventricular Tachycardia
Abstract
ICD is indicated for prevention of sudden cardiac death in patients with cardiomyopathy, given the high risk of ventricular arrhythmia. However, ventricular arrhythmia sometimes caused by the defibrillator itself so that we emphasize to analyze the mechanism of the arrhythmia and deliver an appropriate therapy to patients. We presented the patient who developed episodes of ventricular tachycardia induced by pacing function of ICD. The ventricular tachycardias were terminated once we reprogrammed the ICD pacing function. In conclusion, we emphasize the importance of making correct diagnosis in an individual patient and treatment tailored by the mechanism of arrhythmia.
Core tip
This patient’s ventricular tachycardia represented a paradoxical response from amiodarone administration. It is the reported evidence of MVP-related VT which is very rare incidence [1]. Turning off the MVP and discontinuation of the amiodarone resolved the VT storm.
Introduction
ICD is recommended as a treatment of choice of different kinds of ventricular tachyarrhythmia. However, some pacing function delivered by ICD could potentially initiate a ventricular arrhythmia. Hence, careful analysis the onset and natural history of any ventricular arrhythmia is the key for prevention and treatment [1].
Case presentation
A 75-year old woman with significant past medical history of ischemic cardiomyopathy (ICM) and a survivor of sudden cardiac death (SCD) underwent dual chamber implantable cardioverter defibrillator (ICD) implantation for secondary prevention of SCD. The device (Medtronic Inc. St Paul, MN USA) was programmed to AAI(R)-DDD(R) with managed ventricular pacing (MVP) mode. One year later, during her regular pacemaker clinic visit, the device interrogation revealed atrial fibrillation and she was started on anti-arrhythmic treatment with oral amiodarone. She has been in sinus rhythm since then.
Six months after initiating amiodarone, she presented to the emergency department with shortness of breath and tachycardia. Her blood pressure was stable with no signs of heart failure. Laboratory tests were unremarkable, however12-lead electrocardiogram showed regular wide complex tachycardia consistent with sustained monomorphic ventricular tachycardia (VT). The intravenous amiodarone treatment was initiated. The transthoracic echocardiogram demonstrated severely impaired LV systolic function, similar to the findings from the prior echocardiogram.
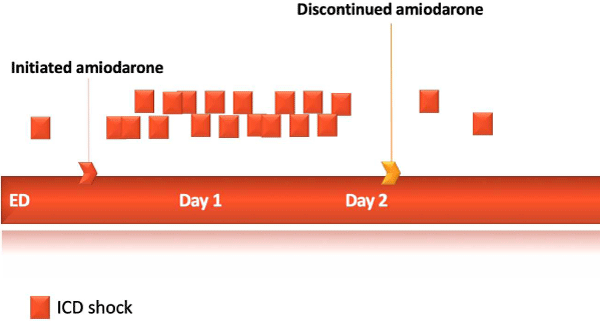
She was admitted to the intensive careand maintained on continuous infusion of the amiodarone. However, even with escalating amiodarone doses combined with intravenous lidocaine, the arrhythmia was not under control, rather, it deteriorated to develop more frequent episodes of VT requiring anti-tachycardia pacing (ATP) and ICD shocks in some cases. We interrogated the telemetry waveforms and were able to deduce a specific initiation pattern for almost every episode of VT. Interestingly, the initiation of arrhythmia was linked to the short-long-short (SLS) sequence created by the MVP-related longer interval of atrial sensed-ventricular paced (As-Vp) beats. The dropped ventricular depolarization followed by ventricular safety pacing induced the VT (Figure 1). Amiodarone also promoted the use of MVP by provoking atrioventricular (AV) conduction delay. Assuming ventricular safety pacing after MVP was the likely initiating factor of VT, we reprogrammed the ICD to turn off the MVP mode, switching to DDDR mode. Additionally, amiodarone and lidocaine were discontinued to lessen the degree of AV conduction delay. Deactivation of MVP and discontinuation of antiarrhythmic agents caused a dramatic improvementin the burden of ventricular tachycardia, substantially reducing the episodes of VT from 34 to 2 events requiring any ATP or ICD shock.
Figure 1: Telemetry illustrated prolong PR interval, atrial paced-ventricular sensing in the upper strip, until non- conducted p wave causing ventricular safety pacing. This dropped ventricular beat caused a long RR interval that was followed by short RR, between VSP and PVC that initiated ventricular tachycardia.
Discussion
Pacemakers and ICDs are approved for various underlying conduction abnormalities and both primary and secondary prevention of sudden cardiac death in patients with heart failure and reduced ejection fraction, respectively. Adverse hemodynamic effects for unnecessary pacing are well established, leading to various manufactured-based various to minimize the pacing. Following the SAVE-Pace trial finding of 40% reduction in the relative risk of persistent atrial fibrillation, the MVP is consistently used in dual chamber devices [2]. Given timely ventricular arrhythmia detection before deteriorating patient hemodynamic, ICD could provide the antitachycardia pacing therapy before more aggressive treatment with ICD shock.
Mechanism of the initiation of the ventricular arrhythmia can point us toward the underlying cause and origin, thereby helping to decide the appropriate management [3]. ICD-related arrhythmia has been presented by many studies in the past [1,4]. In MVP programing, the long-short sequence facilitated by progressive prolongation of native PR interval until loss of AV conduction followed by ventricular safety pacing creates a long RR interval. In this setting, the paroxysmal ventricular contraction (PVC) that can follow the ventricular safety pacing can initiate the sustained monomorphic VT. We emphasize the importance of acknowledging the mechanism of arrhythmia. This patient received the higher doses of amiodarone and even lidocaine which made the MVP effect more frequent due to the worsening AV conduction precipitated by amiodarone. Longer use of amiodarone led to the observation of more episodes of VT due to recurring MVPrelated long-short sequence. Our case presents both the paradoxical response from amiodarone administration in this setting, and, to our best knowledge, it is the reported evidence of MVP-related VT which is very rare incidence [1]. Turning off the MVP and discontinuation of the amiodarone resolved the VT storm.
Conflict of Interest: Dr. John Ip has received research grants from St. Jude Medical, Medtronic and Biotronik. Dr. John Ip has received a speaker honorarium from St. Jude Medical. Other authors declare that they have no conflict of interest.
References
- Fisher JD. Pacemaker pro-arrhythmia: beyond spike-on-T and endless loop tachycardia. J Am Coll Cardiol. 2007; 50: 623-625.
- Sweeney MO, Bank AJ, Nsah E, Koullick M, Zeng QC, Hettrick D, et al. Minimizing ventricular pacing to reduce atrial fibrillation in sinus-node disease. N Engl J Med. 2007; 357: 1000-1008.
- Ulus T, Kudaiberdieva G, Gorenek B. The onset mechanisms of ventricular tachycardia. Int J Cardiol. 2013; 167: 619-623.
- Vlay LC, Vlay SC. Pacing induced ventricular fibrillation in internal cardioverter defibrillator patients: a new form of proarrhythmia. Pacing Clin Electrophysiol. 1997; 20: 132-133.
Citation: Chokesuwattanaskul R, Randhawa MS, Ip R and Ip JH. MVP-Induced Ventricular Tachycardia: Paradoxical Role of Implantable Cardioverter Defibrillator: A Case Report. Clin Cardiol. 2019; 2(1): 1007.
PDF Download